
March 25, 2026
Healthcare
Change Management in Healthcare Software: The Missing Piece of Digital Transformation
Key Takeaways
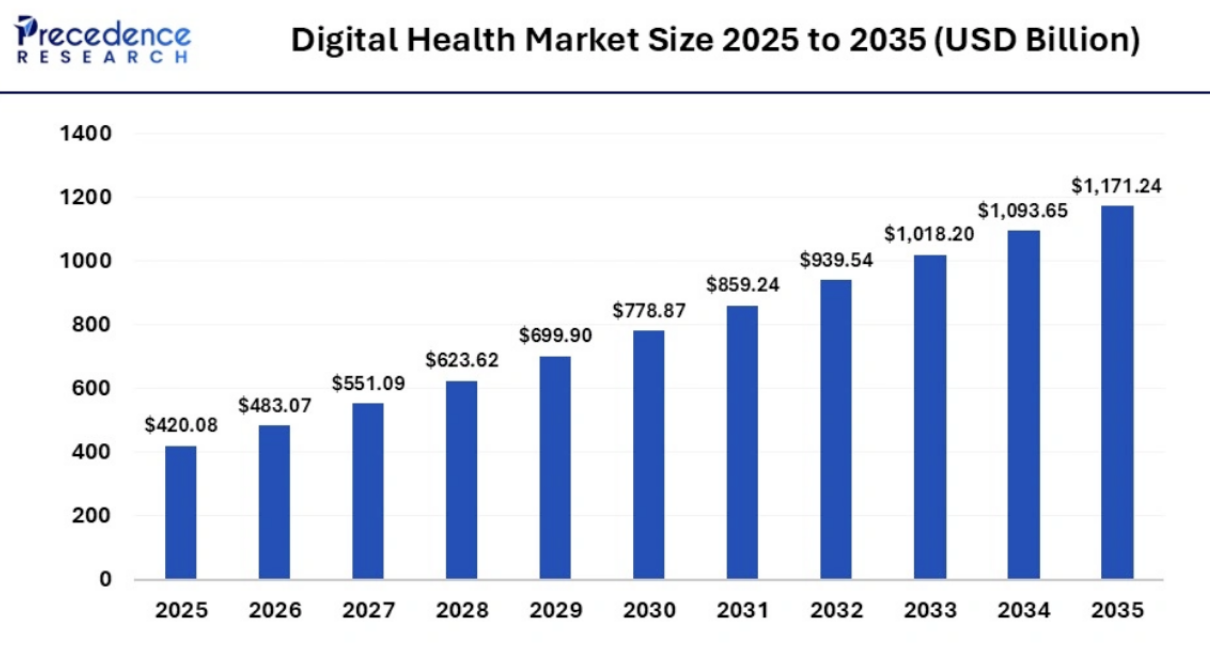 Source: Precedence Research
Source: Precedence Research
A development partner who understands healthcare environments, clinician workflows, HIPAA requirements, healthcare data security, and interoperability standards (HL7 and FHIR) can design software that reduces friction from day one. They build with change management in mind: intuitive interfaces that align with how clinicians already work, phased deployment options, and feedback mechanisms baked into the product.
This is the difference between a system that needs months of workarounds and retraining and one that staff actually want to use. The development partner isn’t separate from the change management process. They’re embedded in it.
EHR integration is a practical example. A partner who has done this before knows the technical migration is only half the job. The other half is helping clinical teams understand what changes in their daily routines, what stays the same, and where to get help when things don’t work as expected. That dual awareness—technical and organizational—is what separates a successful implementation from an expensive underused system.
It also means building digital platforms with adoption in mind from the architecture stage. Healthcare solutions designed with clean, role-specific interfaces, sensible defaults, and minimal clicks to complete core tasks don’t just improve operational efficiency. They reduce resistance from the people who have to use them every day.
- Nearly two-thirds of healthcare change projects fail, and the root cause is almost always people and process, not technology.
- Clinician resistance is a rational response to workflow disruption, not a personality problem. Plan for it.
- Change management is a parallel workstream that runs alongside software development from day one, not a training session a week before go-live.
- Executive and clinical sponsorship is non-negotiable. Without it, initiatives stall.
- Measuring adoption after go-live matters more than the go-live itself.
 Source: Precedence Research
Source: Precedence Research
Why Healthcare Software Rollouts Fail (It’s Rarely the Code)
The People Problem Nobody Plans For
Most healthcare IT project failures don’t trace back to bad engineering. They trace back to people. A well-built system still fails if clinicians weren't prepared to use it, and that puts patient outcomes at risk. According to an HCI Innovation Group, more than 70% of IT projects are deemed unsuccessful, and neglecting human factors in the change management is one of the biggest contributors. Think about what happens in a typical rollout. Leadership signs off on a new platform. The dev team builds it to spec. IT configures the infrastructure. Then someone schedules a two-hour training session, sends a PDF user guide, and calls it done. Nurses and physicians show up to a system they had no input on – one that changes how they document, how they order, and how they communicate—all while they’re already stretched thin. Burnout makes this worse. A systematic review in PMC reports, physician burnout has been increasing across specialties, with nearly 75% of clinicians experiencing burnout symptoms identifying electronic health records as a contributing factor. Burned-out healthcare professionals have no tolerance for poorly introduced digital tools that add friction to their day.Resistance Is Predictable, Not Personal
When clinicians push back against a new system, it’s easy to label that as resistance. It isn’t. It’s a rational response. Clinians have built their workflows around protecting patient care. When a new EHR or scheduling platform disrupts those workflows without adequate preparation, pushback is the natural outcome. Harvard’s T.H. Chan School of Public Health notes that healthcare professionals tend to be exceptional at developing innovative solutions but struggle to implement them, because implementation requires a completely different skill set. The hierarchical nature of healthcare organizations, combined with staff who view their work as a vocation, makes change particularly difficult. Harvard Business Review reinforces the point: clinical and administrative staff are historically suspicious of strategic agendas from senior administrators. Understanding this dynamic is foundational to any healthcare transformation strategy.What Change Management Actually Means in Healthcare Software Development
More Than a Training Session
There’s a common misconception that change management equals a one-day training or a PDF user guide. It doesn’t. Effective change management covers stakeholder alignment, workflow analysis, phased rollouts, feedback loops, executive sponsorship, and post-go-live support. A solid change management plan is a core workstream of any digital transformation healthcare strategy, not an afterthought you bolt on after the code is deployed. treat as one, you get the exact pattern driving those 70% failure rates. Here’s a practical way to think about it: if your project plan has 200 line items for development and testing but only three for “training” and “communication,” change management is underfunded. The ratio should be much closer to balanced, especially in healthcare facilities, where the stakes are higher and the tolerance for disruption is lower than in most industries.The Role of a Healthcare Transformation Strategy
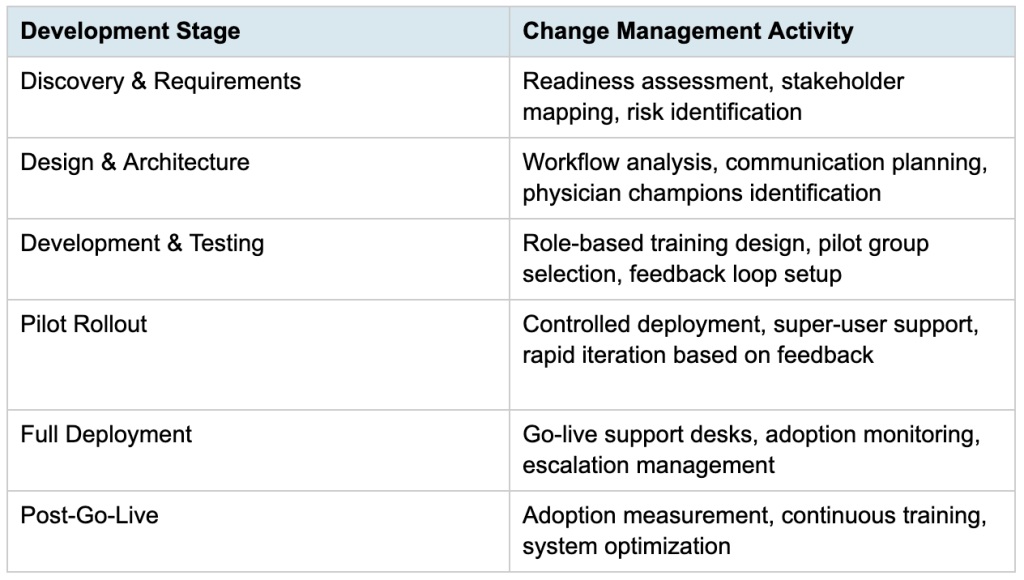
Change management doesn’t exist in isolation. It sits inside a broader healthcare transformation strategy that runs parallel to the software development lifecycle from day one. Here’s a simplified view of how the stages map together:
Change Management Across Common Healthcare Software Types
EHR and EMR Systems
EHR implementations are among the most high-stakes change management scenarios in healthcare. They touch clinical documentation, patient data management, ordering, scheduling, billing, and communication. When a new EHR system goes live, it disrupts almost every clinical workflow in the building. Success requires physician champions who advocate for the system from within clinical teams, not just IT mandates from above. It also requires careful attention to FHIR and HL7 interoperability, which demand parallel change management efforts for both technical teams and clinical staff. Migration from legacy systems means people aren’t just learning a new tool; they’re unlearning years of ingrained habits. And there are real consequences to getting this wrong. According to research published in PMC on EHR-related burnout reports, medical professionals consistently spend twice as much time on electronic documentation and administrative tasks as they do on direct patient care. Nearly 69% of primary care physicians feel that most EHR clerical tasks don’t actually require a trained physician. Inadequate change management only deepens that frustration.Healthcare Supply Chain Management Software
Change management in healthcare supply chain management software development is frequently underestimated. These systems touch procurement, inventory, logistics, and clinical operations all at once. A rollout without proper change management can create stockouts, regulatory compliance gaps, and workflow disruptions across multiple departments simultaneously. The cross-functional stakeholder challenge here is significant – supply chain managers, department heads, clinical staff, finance teams, and regulatory compliance officers, all interact with the system differently and all need to be part of the change plan. A procurement manager cares about vendor integration and cost tracking. A nurse cares about whether the supplies they need are actually on the shelf when they need them. If the rollout team only trains procurement and forgets the clinical side, you end up with a technically functional system that nobody on the floor trusts. In a hospital, the supply chain touches almost everyone — the change plan has to reflect that.Patient-Facing Platforms and Portals
Healthcare digital transformation increasingly includes patient-facing digital solutions: portals, telehealth platforms, mobile apps. Change management here extends beyond staff to patients themselves, and patient engagement becomes a critical success metric. A study published in Frontiers in Communication found patient portal adoption rates have remained stubbornly low, ranging from 37% to 54%, despite the widespread availability of these tools and government incentive programs. That’s a clear signal that technology availability alone doesn’t drive engagement. Onboarding, education, provider advocacy, and patient-centered design are all required. Skip them, even well-built portals go unused. The same dynamic applies to telehealth. Despite heavy pandemic-era investment, adoption has since dropped to around 4–6% of visits, according to CMS and Epic data. The infrastructure exists. The willingness to use it often doesn’t, because patient education and workflow integration were never properly addressed.Building a Change Management Plan That Works in Healthcare
Secure Executive and Clinical Leadership Buy-In First
No change management plan survives without sponsorship from both administrative and clinical leadership –CMOs, CNOs, department heads, and IT directors visibly endorsing and resourcing the initiative. Buy-in isn’t just formal approval. It’s active participation, dedicated resource allocation, and clear accountability structures. The average tenure of a hospital CEO is just 3.5 years, per one Altus analysis. That leadership instability makes long-term change harder to sustain — when a sponsor exits mid-implementation, momentum rarely recovers.Map Workflows Before You Build or Deploy
Software that doesn’t fit clinical workflows gets worked around or abandoned. The best healthcare software solutions start with process mapping, not just requirements gathering. This means sitting with nurses, physicians, billing staff, and administrators to understand how work actually gets done, not how leadership assumes it does. A scoping review on EHR usability challenges published in PMC highlighted that EHR systems frequently require excessive navigation through numerous pages and clicks, pushing clinicians into performing administrative tasks unrelated to patient care. That’s a workflow mapping failure that feeds directly into adoption problems.Train in Context, Not in a Vacuum
Role-based, workflow-integrated training consistently outperforms generic onboarding. Nurses, physicians, billing staff, and administrators all use the system differently. Training should reflect that. What works in practice:- Super-user programs that turn selected staff into in-house experts and peer supports
- Go-live support desks staffed during the critical first weeks
- Hands-on, scenario-based training tied to actual clinical situations, not abstract demos
- Staggered department rollouts so support resources aren’t stretched thin
Measure Adoption, Not Just Go-Live
A successful go-live date is not the same as a successful implementation. Post-launch monitoring is where digital transformation healthcare initiatives either take hold or fall apart. Adoption metrics that matter include:- System login rates and frequency of use by role
- Workflow completion rates – are people using the new process end-to-end?
- Error rates and workaround frequency
- Support ticket volume and recurring issues
- Staff satisfaction scores before, during, and after rollout
The Developer’s Role in Change Management
There’s a persistent idea that the software development partner is just a code vendor: build what's asked, hand over the keys. That model doesn’t work in healthcare.A development partner who understands healthcare environments, clinician workflows, HIPAA requirements, healthcare data security, and interoperability standards (HL7 and FHIR) can design software that reduces friction from day one. They build with change management in mind: intuitive interfaces that align with how clinicians already work, phased deployment options, and feedback mechanisms baked into the product.
This is the difference between a system that needs months of workarounds and retraining and one that staff actually want to use. The development partner isn’t separate from the change management process. They’re embedded in it.
EHR integration is a practical example. A partner who has done this before knows the technical migration is only half the job. The other half is helping clinical teams understand what changes in their daily routines, what stays the same, and where to get help when things don’t work as expected. That dual awareness—technical and organizational—is what separates a successful implementation from an expensive underused system.
It also means building digital platforms with adoption in mind from the architecture stage. Healthcare solutions designed with clean, role-specific interfaces, sensible defaults, and minimal clicks to complete core tasks don’t just improve operational efficiency. They reduce resistance from the people who have to use them every day.
How Kanda Can Help
Effective change management requires a team that understands both the technical build and the organizational reality of deploying software in clinical environments. Kanda has been working in healthcare software development for decades. We can help with:- Assessing your organization’s readiness for a digital transformation initiative and identifying risks before they become roadblocks for your health systems
- Designing and building healthcare software that aligns with clinical workflows, reducing the friction that drives staff resistance
- Handling EHR integration with attention to interoperability standards like FHIR and HL7, so technical complexity doesn’t become a change management bottleneck
- Building phased rollout plans with built-in feedback loops and adoption tracking
- Supporting post-launch optimization so your systems keep delivering value as your organization and healthcare software development trends evolve
Conclusion
Healthcare organizations don’t fail at digital transformation because the software doesn’t work. They fail because no one planned for the human side. Change management is the bridge between a well-built system and a system that actually gets used. It’s the work of mapping workflows before you redesign them, getting leadership genuinely invested, training people in context, and measuring real adoption instead of celebrating a go-live date and moving on. The technology keeps getting better. The budgets keep growing. But none of that matters if the people who are supposed to use the software don’t trust it, weren't trained properly, or were never part of the conversation.Related Articles

CMS Prior Authorization Rule 2026: What Health Systems and Payers Actually Need to Build by October 2027
Key Takeaways The 2026 CMS Prior Authorization (CMS-0062-P) rule extends electronic prior authorization requirements to drugs for the first time, closing a major gap left by the 2024 rule. The hard compliance deadline is October 1, 2027 - by that date, systems must be live, not in development or testing. Compliance requires three major technical…Learn More
Unlocking Actionable Insights from Medical Data with Clinical NLP
Key Takeaways Clinical NLP extracts useful details from notes, reports, and other free-text records so teams can work with them. The clearest use cases include coding support, trial matching, safety monitoring, registry work, and population health. The output is only useful if it connects to the standards healthcare teams already use: SNOMED CT, RxNorm, LOINC,…Learn More
Why Omics and Clinical Data Integration Remain a Challenge and How to Fix It
Key Takeaways Omics and clinical data often remain separate, making them harder to use together than they should be. The main challenge is usually not the data itself, but the mismatched formats, siloed systems, and disconnected teams surrounding it Addressing that requires robust infrastructure, shared standards, and workflows that hold up without constant manual intervention.…Learn More
AI Copilots in Healthcare: Minimizing Diagnostic Risks With Smart Virtual Assistants
Key Takeaways AI copilots act as always-on virtual assistants managing documentation, triage, and decision support so clinicians can focus on patients. With 12 million diagnostic errors and up to 80,000 deaths annually, AI copilots are built to catch what overloaded clinicians miss, not replace them. Dragon Copilot saves clinicians around 5 minutes per encounter with…Learn More

